|
4/17/2017 0 Comments 3 Day Bhf DietCardiovascular Disease Prevention. Observational studies over many decades have shown a close, direct relationship between dyslipidemia and coronary heart disease risk. Intervention trial data collected over the past 2 to 3 decades have also demonstrated that cholesterol modification, especially statin therapy (3- hydroxy- 3- methylglutaryl coenzyme A . The cholesterol- lowering guidelines therefore retain LDL- C as the primary target for lipid modification and statin therapy as the primary means of achieving LDL- C goals. In 1. 98. 8, the first National Cholesterol Education Program (NCEP) was begun in an effort to establish targets for cholesterol levels based on assessments of risk. These guidelines were written by a panel of experts and, in subsequent publications, have been referred to as the Adult Treatment Panel . The NCEP guidelines were evidence based, used CHD risk assessment for the recommended LDL- C targets, and were relatively simple for health care providers, patients, and payers to understand. Over the past 2 decades, the NCEP guidelines have changed in terms of lipid targets based on information obtained from clinical trials and observational studies. You should now be able to take them back to the place where you bought them, supermarkets, also virtually all public buildings in Shropshire have battery recycling. 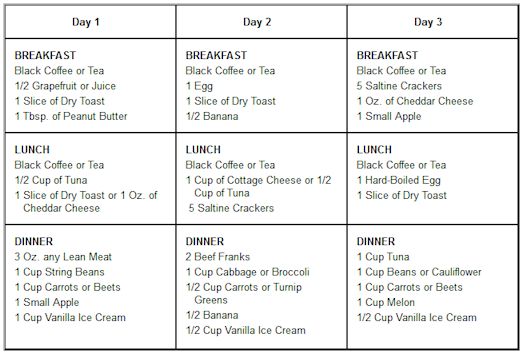  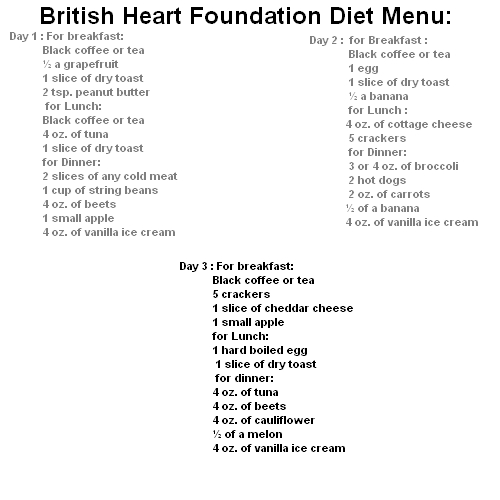
These guidelines have been supported by other organizations, including the American Heart Association (AHA), American College of Cardiology (ACC), American Diabetes Association (ADA), American Association of Clinical Endocrinologists (AACE), and American College of Physicians (ACP). This chapter reviews the history of the guidelines, how new information has resulted in changing targets, and current approaches to CHD risk assessment and gives a summary of approaches to lowering cholesterol. History. The Lipid Research Clinic Coronary Primary Prevention Trial. LDL- C lowering in high- risk men aged 3. At baseline, LDL- C levels were typically in the 1. L range. LDL- C values in the cholestyramine- treated subjects approached the 1. L range. This trial was the foundation for the first set of NCEP guidelines published in 1. CHD who had 2 or more risk factors for CHD have an LDL- C target of 1. L or lower. Lower risk patients with fewer risk factors had correspondingly higher LDL- C targets. The second set of NCEP guidelines, published in 1. LDL- C to . Since the publication of the ATP III, several additional clinical trials of statin cholesterol- lowering therapy were published, leading to updates in 2. In contrast to ATP I and II, ATP III placed greater emphasis on the prevention of CHD in patients with multiple risk factors, in addition to treatment for secondary prevention. The ATP III treatment algorithm divided patients into 3 risk categories based on clinical characteristics and the Framingham 1. Established CHD and CHD risk equivalents: High risk (1. Multiple (2 or more) risk factors: Moderately high risk (1. Zero to 1 (1 or none) risk factor: Lower risk (1. ATP III greatly expanded the high- risk category by defining CHD . ATP III major risk factors include the following: Age (men, 4. According to National Health and Nutrition Examination. Heart Month 2017: Here. With February declared Heart Month, many countries and organisations around the world. Just what I had thought, so pleased that I am normal, all my bloods are normal, I eat a healthy diet and took myself off statins, my cholesterol was 7.8. Open heart surgery is performed in order to repair a fault or damage in the heart. Learn all about what happens and what the recovery process is like. As previously stated, patients with type 2 diabetes mellitus can usually be differentiated from those with type 1 disease on the basis of history and physical.Cigarette smoking. Hypertension (blood pressure = 1. Hg or patient is on antihypertensive medications)Low high- density lipoprotein (HDL) cholesterol level (< 4. L in men, < 5. L in women; HDL cholesterol . For all patients in the high- risk category with LDL- C > 1. L, LDL- C- lowering dietary therapy should be initiated. In addition, for patients with LDL- C > 1. L, an LDL- C- lowering drug should be started. However, in the LDL- C range of 1. L, ATP III guidelines did not mandate drug therapy; rather, therapeutic options included intensified dietary therapy, LDL- C- lowering drugs, or drug therapy for elevated triglyceride or low HDL- C levels. At the time of publication of the guidelines for ATP III, there were not enough data to recommend more intensive drug therapy for this intermediate range of LDL- C. These recommendations were modified in the ATP III update of 2. LDL- C goal < 1. L for high- risk patients, with an optional goal of < 7. L for very high- risk patients (Table 1). This update also recommended initiating dietary therapy and LDL- C- lowering drugs for all patients over goal, with a planned LDL- C reduction of 3. The rationale for these changes was based on several randomized clinical trials, the results of which were published after the release of the ATP III guidelines. Table 1. Summary of ATP III Guidelines Update, 2. Risk Category. LDL- C Goal. Initiate TLCConsider Drug Therapy. High risk. CHD or CHD- risk equivalent(1. L; optimal goal, < 7. L. Implications of recent clinical trials for the National Cholesterol Education Program Adult Treatment Panel III Guidelines. Patients treated with simvastatin had a 2. LDL- C < 1. 00 mg/d. L. The Pravastatin or Atorvastatin Evaluation and Infection- Thrombolysis in Myocardial Infarction 2. PROVE IT- TIMI 2. Ultimately, it showed that intensive LDL- C level lowering with atorvastatin 8. The mean LDL- C level attained was 9. L with pravastatin and 6. L with atorvastatin. The study demonstrated a 1. P < 0. 0. 05). Other trials used to support these revised guidelines included the Prospective Study of Pravastatin in the Elderly at Risk (PROSPER),1. Antihypertensive and Lipid- Lowering Treatment to Prevent Heart Attack Trial- Lipid- Lowering Trial (ALLHAT- LLT),1. Anglo- Scandinavian Cardiac Outcomes Trial- Lipid- Lowering Arm (ASCOT- LLA),2. Finally, in the evolution of the cholesterol guidelines, the AHA/ACC guidelines for secondary prevention of CHD released in 2. LDL- C < 7. 0 mg/d. L in high- risk patients with CHD, based on data accrued from the Treat to New Targets (TNT) and Incremental Decrease in Endpoints through Aggressive Lipid Lowering (IDEAL) trials. It was formulated as a Class IIa recommendation and stated that it is reasonable to treat to LDL < 7. L in such (secondary prevention) patients. When the < 7. 0- mg/d. L target is chosen, it may be prudent to increase statin therapy in a graded fashion to determine a patient’s response and tolerance. Furthermore, if it is not possible to attain LDL- C < 7. L because of a high baseline LDL- C, it generally is possible to achieve LDL- C reductions of > 5. LDL- C- lowering drug combinations. Back to Top. Risk assessment. Several variables have been taken into consideration to determine CHD risk. Any patient who has had a CHD event is at markedly increased risk for a subsequent event. Risk models such as the Framingham risk score. Any patient who has a > 2. CHD event based on the Framingham risk score is considered to be at equivalent risk to a patient with established CHD. The Framingham risk score does not take into account family history because of difficulty obtaining this measure in all patients. Furthermore, it does not include some of the newer markers such as high- sensitivity C- reactive protein (hs. CRP) or microalbuminuria. Current guidelines and many clinical studies consider diabetes mellitus as a CHD risk equivalent (> 2. LDL- C and non. Low HDL- C concentrations are associated with increased CHD risk. Studies such as AFCAPS/TEXCAPS have demonstrated that aggressive LDL- C lowering attenuates much of the adverse risk associated with low HDL- C. There are also extensive data showing that hs. CRP is associated with increased risk for CHD, even when adjustments are made for other risk factors. Current guidelines suggest that hs. CRP be used to help in ongoing risk assessment in patients judged to be at intermediate risk for CHD. In fact, the Reynolds Risk score is one such risk assessment tool that incorporates hs. CRP as well as family history of CHD in parents at age < 6. This risk calculator is modeled to project lifetime CHD risk, and may be useful for assessment of risk in women, for whom the Framingham score often tends to underestimate risk. Other markers of risk have not been consistently included in guidelines but should be considered in clinical practice. Renal dysfunction is associated with an increased risk for CHD. This is true for markers of renal disease such as albuminuria, but several studies have shown that impaired renal function is associated with marked increases in CHD risk, especially when associated with the need for renal replacement therapy (dialysis or renal transplantation). Peripheral vascular disease and cerebrovascular disease are also associated with increased risk for CHD events. Furthermore, most statin trials have shown a reduction in risk for stroke, although stroke event rates are consistently lower than CHD event rates in most studies. Several observational studies have suggested that patients who have systemic inflammatory disorders such as rheumatoid arthritis and systemic lupus erythematosus, especially if they are treated with glucocorticoids, are at increased risk for CHD. Similarly, organ transplant recipients, especially renal, heart, and lung transplants, may be at increased risk for CHD. Many CHD risk prevention clinics, including the Preventive Cardiology Clinic at the Cleveland Clinic, have set more aggressive LDL- C targets for such patients. This approach extends the general concept of more aggressive lipid lowering in patients at increased risk of disease. Back to Top. Lipid- lowering treatment. Diet and Lifestyle. All patients, whether in secondary or primary prevention categories, are urged to implement lifestyle and dietary strategies to prevent cardiovascular disease. Healthy eating habits, starting in childhood, are the cornerstone for cardiovascular risk reduction and, together with lifestyle goals, including maintenance of healthy body weight, avoidance of tobacco products, and adherence to a regimen of physical activity, may be termed elements of primordial prevention. Specifically, the American Heart Association recommends a diet low in fat, particularly saturated and trans fats, enriched in fruits, vegetables, whole grains, and fish, and low in added sugar and salt (Table 2). This approach, especially regarding fat intake, is supported by other nutrition guidelines. Why hasn’t my healthy diet cut my cholesterol? Here’s an extract (in blue) from my book The Obesity Epidemic: What caused it? How can we stop it?“The average cholesterol levels for England were reported by the National Health Service (NHS) as 5. L for men and 5. 6 mmol/L for women. I found the BBC statement of the position statistically implausible: ? Even if we get into the detail of the mean, median and mode, surely the average for a data group defines normal for that data group. The notion that an actual norm is somehow abnormal . The normal distribution curve sets a norm by definition. For us to declare the actual cholesterol norm to be abnormal, is not normal in itself. This would be like suddenly declaring normal blood pressure to be 1. In the Western Journal of Medicine, (May 2. Thomas Samaras and Harold Elrick posed the question . The table had the following height orders (tallest first): African Americans; White Americans; Hispanics; Asian Indians; Chinese and Japanese (the first two groups were recorded as of equal average height . The age standardised death rates for all causes and coronary heart disease were included in the table. A clear pattern was immediately obvious. I calculated the correlation coefficients as 0. CHD and 0. 9 for height and all causes of death. What if we concluded that height were a cause of CHD (and all causes of death) and that we should therefore redefine the average height to declare the actual average of 6. American men) to be abnormal. What if we picked an arbitrary new target 1. L is approximately 1. L) and decreed that normal height should be approximately 6. We could then stop the body from performing a normal bodily function (growth) by administering drugs to stop growth hormones from doing their job. I trust that this analogy disturbs you. The Chinese practice of foot binding . Cholesterol in the diet doesn’t matter at all unless you happen to be a chicken or a rabbit.”)Dr Scurr says: “This, as you know, is a frustrating situation, and is due to the liver naturally producing too much cholesterol.”The body is designed to produce cholesterol. Not only the liver produces cholesterol – every cell of the body produces cholesterol. This is because cholesterol is so utterly vital for human life, we die instantly without it, that the body must have fool proof mechanisms for making cholesterol. Dr Scurr says: “Although we do get cholesterol from food, most is made by the liver, and it is our intake of foods high in saturated fat that is thought to increase levels of ! How many things can a doctor get wrong in one sentence: a) There’s no connection whatsoever between cholesterol in food and cholesterol in blood and we’ve known that all along. LDL stands for Low Density Lipoprotein. LDL is not cholesterol, let alone bad. LDL carries cholesterol and protein and triglycerides and phospholipids. How a carrier of four substances ends up being called one of them, I know not. LDL is the residue of IDL (Intermediate Density Lipoprotein); IDL is the residue of VLDL (Very Low Density Lipoprotein). LDL, IDL and VLDL are all lipoproteins (think of lipoproteins as . Another lipoprotein (the largest) is called a chylomicron and this transports dietary fat from the digestive system around the body to do its vital work. How any dietary fat, saturated or otherwise, leaps out of chylomicrons and finds its way into VLDL and then IDL and then LDL “to cause havoc in blood cells” is not only unexplained, it is ludicrous! The most interesting bit in the sentence is “we are still unclear exactly how it does this.” Quite so! Not only is there no evidence that dietary fat does impact LDL, there is no understanding of how exactly it can! Dr Scurr says: “Treatment with a statin to lower your cholesterol level might be advisable. Statins do not save lives in women. Statins do not save lives in women. Is it possible to highlight how important this fact actually is? Statins do not save lives in women.”Susan needs to know what statins actually do in the human body. The body is designed to produce cholesterol. Human life depends on the body doing this. Statins impair the body from producing the cholesterol it was designed to make. Thankfully statins don’t work fully, or they would have a 1. Statins block something called the mevalonate pathway. Blocking the mevalonate pathway means that no cell can replicate or repair itself. Blocking the mevalonate pathway means that every cell in the body dies. The only thing that varies is how long each cell takes to die . You do not want to lower your cholesterol level in any circumstances. You may like to look at the graphs on this blog – I have done some original research with all the World Health Organisation data available for 1. It shows that (read this carefully) the lower the cholesterol levels the higher the death rates from heart disease and all causes of mortality for both men and women; the higher the cholesterol levels the lower the death rates from heart disease and all causes of mortality for both men and women. Cholesterol is utterly life vital. We die instantly without it. We need it for every single cell of the body, the muscles, the brain, hormones, bile production, fat digestion, reproduction . This makes cholesterol even more vital to the body than essential fats and protein . If you were to get pregnant, your body would make extra cholesterol because you need lots of cholesterol to make a healthy baby. If you had an operation or an injury, your body would make extra cholesterol to repair you – because that’s what cholesterol does – repair you. One statin alone, Lipitor, has been worth $1. Pfizer since 1. 99. It is not the only statin. There is huge financial benefit to statin manufacturers to try to artificially lower your cholesterol level. There is likely no benefit to you and substantial harm. Statins stop the body from making the cholesterol that it was designed to make (not entirely, or they would have a 1. Statins block something called . Blocking the mevalonate pathway means that no cell can replicate or repair itself. Blocking the mevalonate pathway means that every cell in the body dies. The only thing that varies is how long each cell takes to die . Walking is also an excellent activity to have chosen – natural and enjoyable and this should have given you further health benefits. Red meat from grass living animals is the healthiest food that humans can consume. It’s what we evolved to eat. Giving this up will have worsened your health and you may have lost vital complete proteins, essential fats, vitamins and minerals as a result. Giving up any processed food (including processed meat, which sausages and bacon tend to be) is always a good idea. Cheese is a vital source of calcium, phosphorus and magnesium (the bone nutrients, so vital for women to avoid osteoporosis), as well as fat soluble vitamins and protein, hence your health may also have suffered as a result of this random decision. Oily fish actually has more fat overall and more saturated fat than red meat (Ref 5). Not that any natural dietary fat is bad for you, but just to point out that you may not have achieved what you set out to achieve for whatever misguided reason. The only bad fat is the one made by man and found in margarines, spreads and many processed foods. Do not worry about your cholesterol level. You should revere, not fear, cholesterol. The average GP knows frighteningly little about cholesterol, as Dr Scurr has illustrated. The Hippocratic oath taken by doctors is “First do no harm. In my opinion, doctors administering powerful drugs to stop your body doing what it was designed to do and to block the mevalonate pathway is not only in breach of the Hippocratic oath, it is medical malpractice. Very best wishes – Zo. Her life could literally depend on it..
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. Archives
November 2017
Categories |
 RSS Feed
RSS Feed
